Introduction
The old adage of ‘see one, do one, teach one’ is a relic from a past era of surgery and current residents are learning in the era of outcomes and evidenced based medicine. This is in part due to an evolution our understanding of skill acquisition and surgical education. Furthermore, it is in response to duty hour restrictions, the COVID-19 pandemic and patient safety concerns.1,2 Thus, significant advances to supplement surgical education have been made. The traditional cadaveric dissections,3,4 animal models, 3D printed models, virtual reality (VR) and augmented reality (AR) all have roles in surgical education in the current paradigm.
However, the ability to teach and assess the acquisition of surgical skill has been thought to be the least standardized component of residency education.5 Emphasis is now being placed on quantitative assessment of a uniform skill set using standardized metrics for particular procedures.6 Simulation in all forms has the ability to expose residents in various fields to open, endovascular and minimally invasive techniques.7 In fact, the Accreditation Council for Graduate Medical Education (ACGME) and the American College of Surgeons strongly support the use of simulation in surgical training and to obtain board certification in general surgery, residents must complete a full simulation training in laparoscopy.8 In neurosurgery, the Congress of Neurological Surgeons established a simulation committee and noted that each module in vascular, spine or cranial models improved didactic and technical skills within the framework of the ACGME core competencies.9 However, individual learners bring different skill sets and limitations and thus a tailored approach within the realm of evidence-based standardization is required.10 The ultimate test of successful simulation in any form is to show a positive influence on patient outcomes. One systematic review of 30 RCTs showed that that model, cadaver and video simulation all have benefit for the learner.11
Ensuring that trainees have access to a dedicated learning space that is equipped to provide supplementation to traditional learning in the operating room with cadaveric, 3D printed, and VR technologies with a varied but consistent exposure to surgical techniques is paramount. Incorporating objective, reliable and validated forms of assessment during these trainings is also important such as the objective structured assessment of technical skill (OSATs),12 Global Rating Scale,13,14 direct objective metric tools,15,16 and video recordings.17 While the abilities of machine learning and AI are advancing in assessing performance, teaching surgical skill, and, importantly, surgical decision making still decidedly rests in the hands of the experts in the fields.10 In fact, residents have reported a low satisfaction regarding their training when there is limited access to simulation but even more importantly when this is in conjunction with a lack of teachers.18,19 A dedicated space that can incorporate the human element, AI, various simulation modalities, and allow for both individual and standardized learning is the ultimate goal. We report our institutional experience with designing a surgical training laboratory that serves to harmoniously incorporate the two and remain relevant for the 21st century.
Institutional Experience
Lab Design
In considering the features of the optimal surgical training laboratory, we draw from our own experiences constructing a multi-modality lab. We condense our experience to three core principles that will ensure the surgical teaching lab will remain relevant and highly utilized well into the 21st century including connectivity, integration of learning modalities, and an open concept design.
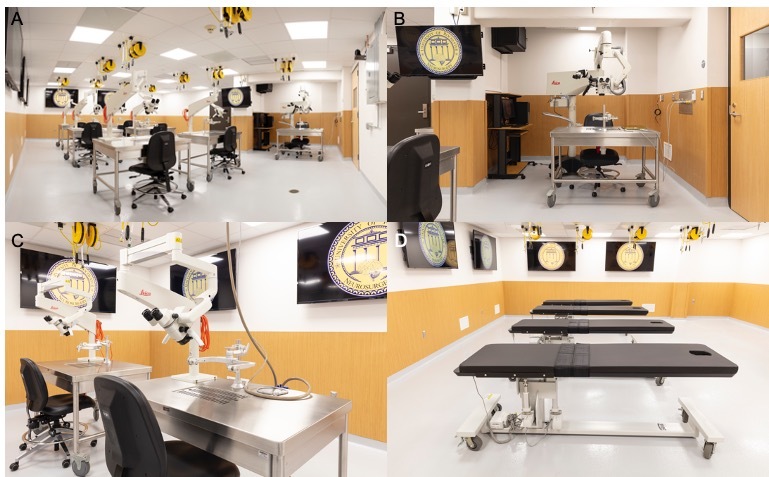
The first of the core principles is connectivity and integrated telecommunications infrastructure. As the Covid-19 pandemic has shown us, the future will be based on being able to connect broadly through televideo means.20 Labs should be designed with the ability to receive input from any source, globally, and easily display that within the facility. Similarly, activity within the lab should be easily captured and broadcast broadly with high fidelity. The telecommunications infrastructure must be adaptive, allowing for easy removal and upgrade, in order to accommodate future developments. In addition, a centralized computer hub should be present in every such facility. This prosector station will allow for seamless utilization of all telecommunication and visual-audio capabilities (Figure 1b). Additionally, the prosector station should be able to run programs needed for functioning of the simulators and should have connectivity capabilities to display the activity throughout the lab. We have incorporated six 65 inch, ultra-high definition screens and 4K audio throughout the lab which communicate with a prosector station. Any connection through the prosector station can thus be broadcast throughout the lab, be it microscope view, VR headset views, or external conference. In fact, we are now using remote proctoring technology to have otherwise unavailable experts teach residents and faculty within the lab from a remote location using these technologies.
Another principle of future surgical teaching facilities is an ability to seamlessly integrate all learning platforms.21 This means that the lab should be designed to accommodate cadaveric, animal, 3D-printed, and simulator models. Many states and countries have specific regulations for working with cadaveric and animal specimens. Airflow turnover, sterility, storage, and designated preparation areas need to be considered prior to embarking on construction of such a facility (Figure 2b). The lab at the University of Rochester has been designed to have the highest air-turnover in the university. All rooms are also equipped with eyewash stations and other safety features.
The final core principle of the facility is an open concept design. The main teaching space should be open without any fixed tables, chairs, or other structures, allowing for new technologies or special equipment to be brought in for each specific course. Any utility ports including irrigation, suction, and power should be placed out of the way but easily accessible (Figure 1a). Our laboratory features six mobile custom designed cranial stations each with a mounted microscope, four spinal stations and a prosector cranial station with a high-end operative microscope with 4K video recording capabilities (Figures 1c, 1d). There are four additional storage rooms, an administrative office and a resident office. Two storage rooms are directly attached, with one designed for instrument storage and the other for instrument processing (Figures 2a, 2b). Two larger storage rooms are for equipment and table storage including custom designed cranial and spinal tables, C-arms, lead aprons, endoscopic towers (Figures 2c, 2d). In total, we have 1846 square footage of space, 933 square feet of the primary lab space and 913 square feet of storage and office space.
It is important to note that the main barrier to development of a multi-modal training labs such as this is cost. However, a lab such as this serves as a venue for both the medical school and many surgical departments. It also acts as a setting for each institution to hold courses at the regional and national level for decades. Thus, with institutional, alumni, and industry support, such a facility becomes quite feasible. In our experience, we have been able to secure approximately $550,000 from industry and an additional $500,000 from alumni.
Lab Curriculum
From November 2020 to May 2023, we have had 43 skills labs for residents and 2 labs for medical students interested in neurosurgery, totaling approximately 1.4 labs per month. Of these, 21 focused on cranial approaches, 22 on spine and 4 on peripheral nerve (PNS). Industry sponsored 20 labs and were split between 16 companies. Of our labs, 30 utilized cadaveric models, 15 3D printed simulators, 3 animal models and 2 with supplemented augmented reality. Our lab is managed by a full-time staff member who maintains the stock of surgical equipment, organizes visiting professorships, coordinates vendor’s supplies and interfaces with the residents.
Labs are currently based on specialty interest of visiting professors and faculty neurosurgeons, as well as requests by industry, including 17 different companies. We have developed a skull base curriculum with the goal of expanding this curriculum to cover all subspecialties of neurosurgery. This was possible after securing high quality injected and preserved cadaveric heads. Residents, a junior and senior are paired with a faculty member and perform dissections on their own pace with periodic check-ins by faculty. As previously mentioned, the limitation to learning is the access to teachers and the success of such a lab requires commitment to education from departmental leadership and faculty. We have had 13 visiting professors and the remaining 28 labs were hosted by internal URMC faculty.
Future Directions/Limitations
Next steps in our program are to establish a proficiency-based methodology as a core curriculum in addition to the programming currently offered. Additionally, with each instructional lab offered, the possibility for repeated measures and self and expert assessment should be the goal. Finally, we must adapt our training with the continually changing landscape of surgical simulation technology specifically with AR, machine learning and VR.
Conclusion
As more attention is focused on training outside of the operating room, the surgical lab remains the most viable method currently available for surgical rehearsal. We believe that a surgical laboratory that facilitates learning in any classical or investigational method can produce superior results compared to labs constrained by layout or technological capabilities while drawing upon the benefits of each method of education. Any such laboratory should rely on the three core principles of connectivity, multiplatform integration, and a dynamic open concept. While it represents a large upfront investment, a technologically advanced multi-modal laboratory can serve as a central educational hub for all surgical specialties at an academic center.
Ultimately the surgical education of the future will be an amalgamation of the modern and traditional methods. The future of surgical education across specialties will no doubt involve surgical simulation that include multiple modalities with standardized assessments. Ideally, these would evolve into a core curriculum for all trainings programs across the country within a specialty with supplementation for the particular needs of that program as necessary. Building spaces that can forward progress to this goal within training programs is critical. Every medical school and surgical training program should continue to endeavor in developing a space where learners can see, do and teach many with expert supervision, standardized assessment tailored to individuals and with a focus on patient outcomes.
Acknowledgements
We would like to thank Melanie Zandvoort, Babak S. Jahromi, Shirley A. Joseph, Arlene and Norman Leenhouts, Judy and Paul Linehan, and Kevin J. Mullins for their contribution and support.